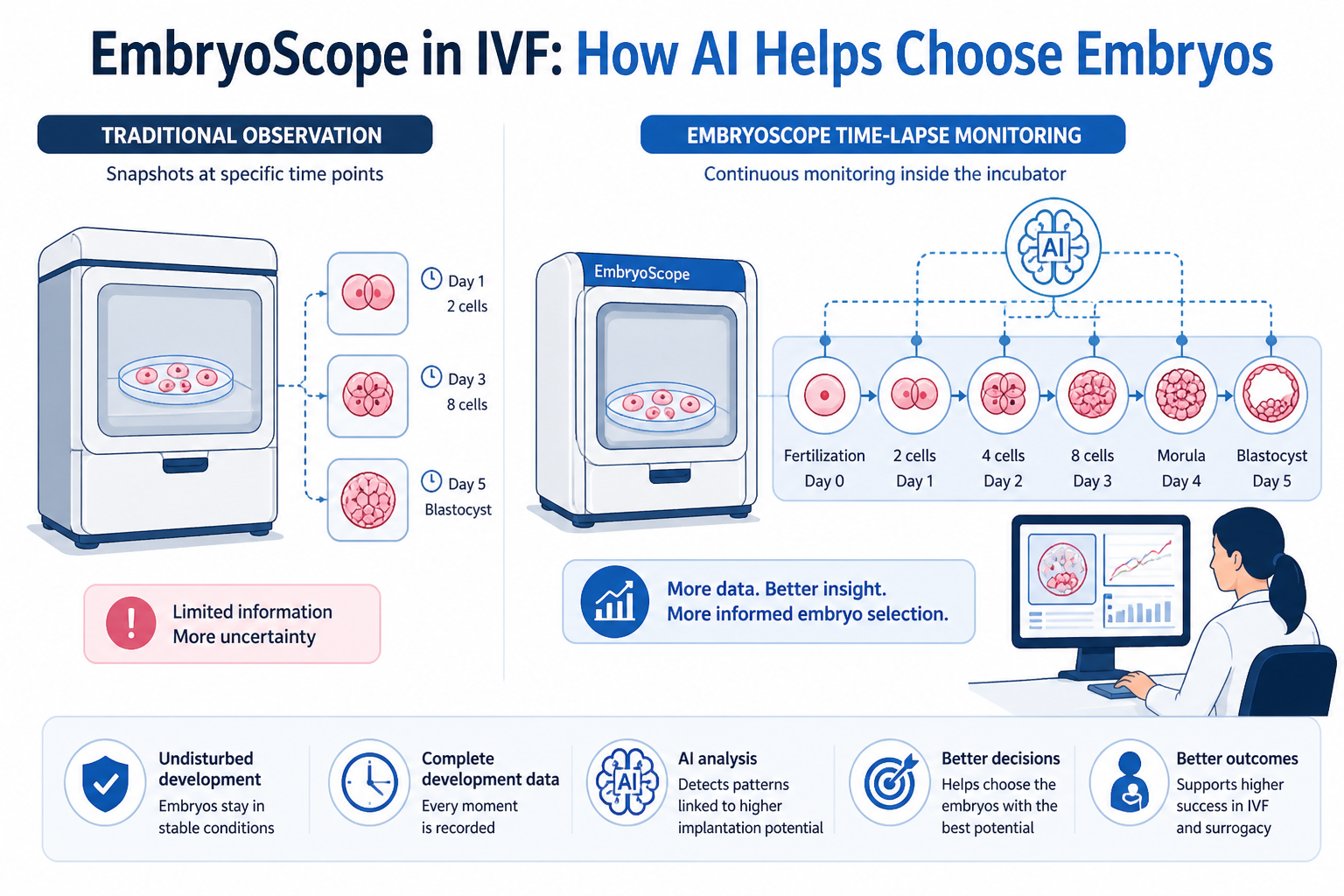
Choosing which embryo to transfer is one of the most important decisions in IVF, especially when a surrogacy program depends on each attempt. Patients coming to SILK Medical often ask how doctors decide between embryos that may look similar at first glance. Traditional methods rely on brief observations at specific time points, which leaves gaps in how development is understood.
Newer systems like EmbryoScope approach this differently by tracking embryo development continuously inside the incubator, giving embryologists a much more detailed picture of how each embryo grows before transfer.
What EmbryoScope actually is
EmbryoScope is an incubator with a built-in camera system that records embryo development without removing embryos from a controlled environment. In a standard lab setup, embryos are taken out at specific times for observation under a microscope. With EmbryoScope, images are captured every few minutes, creating a full time-lapse sequence of how each embryo develops from fertilization to the blastocyst stage.
This matters because embryos remain undisturbed. Temperature, gas levels, and humidity stay stable, which supports more consistent development while still giving embryologists detailed visual data.
How AI is used in embryo assessment
The AI component works on top of the time-lapse data. It analyzes patterns such as the timing of cell divisions, symmetry, and developmental milestones. These patterns are compared against large datasets of previous IVF outcomes (PubMed study).
The system does not replace the embryologist. It highlights embryos that follow development patterns associated with higher implantation potential. The final decision still comes from the medical team, but it is based on more structured and complete information than visual checks alone.
Why continuous monitoring changes the picture
With traditional observation, embryologists see embryos at selected time points. Two embryos might look similar at a specific moment, even if their development paths were very different.
Time-lapse monitoring fills in those gaps. It shows whether cell divisions happened at expected intervals, whether development was smooth or irregular, and whether there were subtle delays that would not be visible during a single check. This added layer of detail helps distinguish between embryos that appear similar on the surface.
How EmbryoScope works together with PGT-A
EmbryoScope evaluates how an embryo develops. PGT-A testing looks at whether the embryo has the correct number of chromosomes. These are different types of information.
In practice, they complement each other. PGT-A helps identify chromosomally normal embryos, while EmbryoScope helps prioritize which of those embryos may have stronger implantation potential based on development patterns. Many IVF programs combine both approaches when patients want a more precise selection process.
Why this matters in surrogacy programs
In surrogacy, each embryo transfer involves preparation of the surrogate, coordination of medical timelines, and legal steps. Reducing the number of unsuccessful transfers can make a real difference in how long the process takes and how predictable it is.
More informed embryo selection helps avoid transferring embryos that have lower chances of implantation. This can shorten the overall timeline and reduce the need for repeated preparation cycles for the surrogate.
Who benefits most from this approach
Time-lapse monitoring and AI-assisted assessment are especially useful in cases where embryo selection is less straightforward. This includes patients with previous IVF failures, inconsistent embryo development, or limited numbers of embryos.
It is also relevant for donor egg programs and surrogacy cases, where the goal is to make the most efficient use of each transfer attempt.
EmbryoScope at SILK Medical
SILK Medical uses time-lapse monitoring with EmbryoScope as part of its IVF programs. The system works alongside other lab technologies, including PGT-A genetic testing and the IVFID Witness system, which tracks biological samples throughout the process to avoid any mix-ups.
These tools are integrated into standard laboratory workflows rather than offered as add-ons, which allows for consistent embryo assessment across different types of IVF and surrogacy cases.
What AI does not do
AI does not predict pregnancy with certainty, and it does not replace clinical judgment. It does not change the genetic makeup of an embryo or compensate for underlying medical factors.
Its role is to improve how embryos are evaluated by using more data than was previously available. The outcome still depends on multiple factors, including uterine conditions, overall health, and the quality of the genetic material.
How better embryo data changes IVF decisions
Embryo selection has always been a key step in IVF, but the way it is done has shifted with access to continuous data. Instead of relying on a few visual checkpoints, embryologists can follow the full development pattern of each embryo and compare it against known outcomes.
This approach is part of how IVF and surrogacy programs are planned from the start at SILK Medical. More detailed embryo data helps structure transfer decisions more carefully, which can reduce unnecessary attempts and make the overall process more predictable for patients.